📋 Quick Navigation
Welcoming a newborn into the world is a joyous occasion, but sometimes babies need extra support right after birth. This is where specialized care units come in, providing a safe haven for fragile infants. In this guide, we'll explore what is nicu, its role in newborn health, and how different care levels ensure every baby gets the attention they deserve. Whether you're an expectant parent or simply curious, understanding these aspects can bring peace of mind.
Understanding the NICU: A Lifeline for Newborns
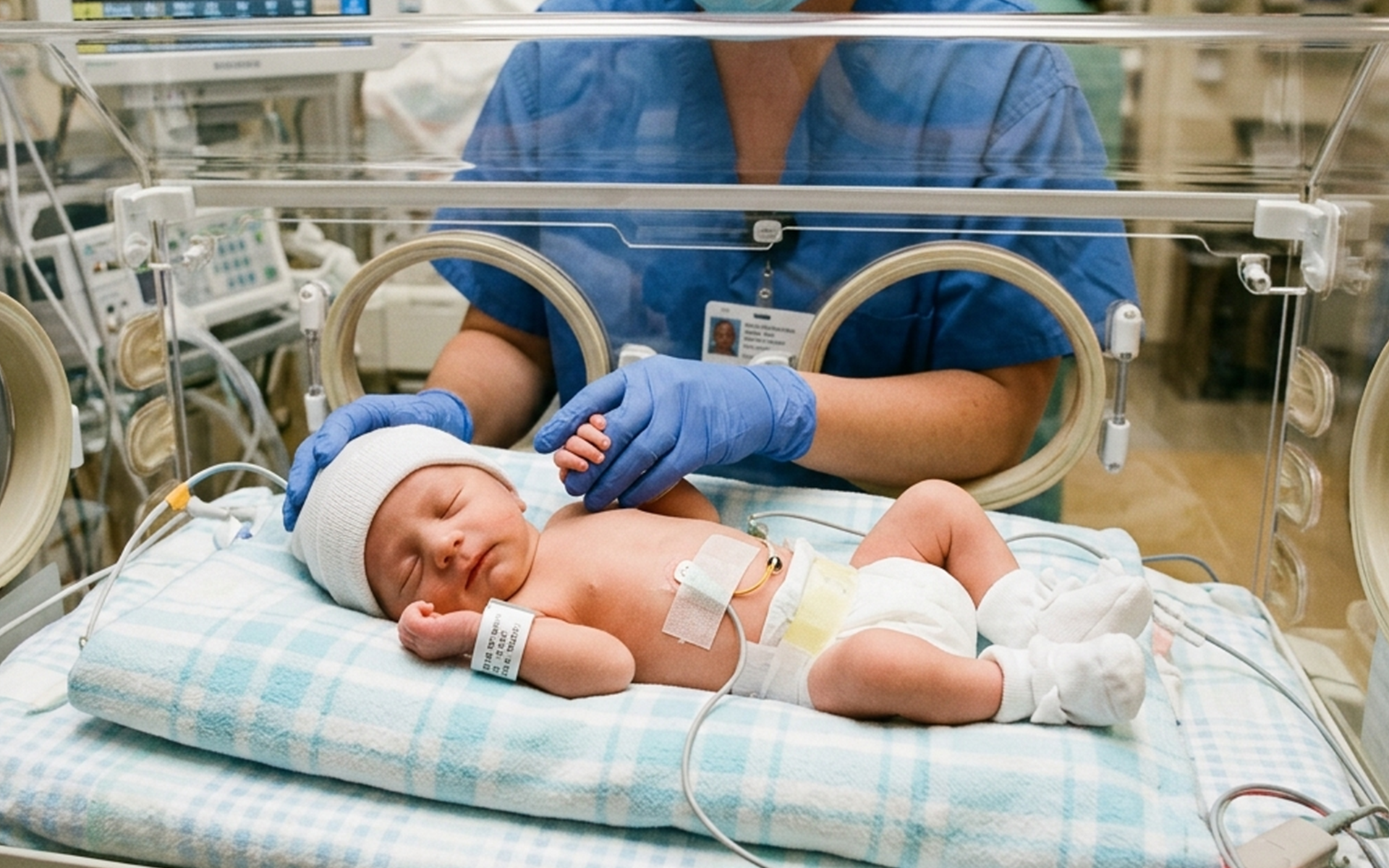
The NICU full form is Neonatal Intensive Care Unit. It's a dedicated hospital area equipped with advanced technology and expert staff to care for premature, low-birth-weight, or ill newborns. The NICU room is designed like a high-tech nursery, featuring quiet lighting, temperature controls, and monitoring systems to mimic a womb-like environment. Each NICU bed often includes incubators or warmers that regulate body heat, protect against infections, and support vital functions.
In the NICU, babies receive round-the-clock monitoring for breathing, heart rate, and other essentials. This setup helps infants who face challenges like respiratory distress, jaundice, or congenital issues to stabilize and thrive.
NICU and the Different Levels of Neonatal Care
| Level | Description | Suitable For | Key Features |
|---|---|---|---|
| Level I (Well Newborn Nursery) | Basic care for healthy or mildly ill full-term babies. Focuses on routine check-ups, stabilization, and minor treatments like jaundice management. | Babies born at 35-37 weeks or later with no major issues. May transfer to higher levels if needed. | Pediatricians, nurses; basic equipment like warmers and oxygen. |
| Level II (Special Care Nursery) | Intermediate care for moderately preterm or sick infants. Includes short-term ventilation and feeding support. | Babies born after 30 weeks, weighing under 1500 grams, with issues like apnea or feeding difficulties. | CPAP machines, incubators, monitors; staffed by neonatal nurses and pediatricians. |
| Level III (Neonatal Intensive Care Unit) | Advanced care for very premature or critically ill newborns. Offers full life support and specialist consultations. | Infants under 30 weeks or below 1200 grams, with severe respiratory or cardiac problems. | Ventilators, infusion pumps, imaging like MRI; team includes neonatologists, surgeons, and ophthalmologists. |
| Level IV (Regional NICU) | Highest level for the most complex cases, including surgeries and rare treatments. | Babies needing ECMO (heart-lung bypass) or repairs for birth defects. | All Level III equipment plus surgical suites and transport services; full pediatric specialist team. |
Not all newborns require the same intensity of care, which is why hospitals offer varying levels of neonatal care. These levels of newborn care are classified based on the baby's needs, gestational age, weight, and health complications. They range from basic support to highly specialized interventions, ensuring efficient resource use and optimal outcomes.
Here's a clear breakdown of the four main levels:
These levels help match care to the baby's condition, promoting faster recovery and reducing unnecessary transfers.
Key Differences in Neonatal Units
Parents often wonder about the difference between SNCU and NICU and PICU. SNCU (Special Newborn Care Unit) is similar to a Level II nursery, providing intermediate care for stable but vulnerable infants, like those with mild infections or prematurity. In contrast, NICU typically refers to Level III or IV units for intensive, life-saving interventions. PICU (Pediatric Intensive Care Unit) is for older children (usually over 1 month) with critical illnesses, not newborns. Knowing these distinctions can help families navigate hospital options effectively.
Admission of Neonates to the NICU
The admission of neonates happens when a baby shows signs of distress or vulnerability post-birth. Common reasons include:
Prematurity (before 37 weeks)
Low birth weight
Breathing problems or apnea
Infections, jaundice, or heart defects
Complications from maternal health issues like diabetes or hypertension
Multiple births or IVF conceptions, which increase risks
Upon admission, doctors assess the infant and assign the appropriate level. The process is swift to ensure immediate support, with parents often involved in updates and decisions.
NICU Baby Care: Nurturing Fragile Lives
Nicu baby care goes beyond medical treatment; it's about holistic support for growth. Specialized teams monitor vital signs, administer nutrition via tubes if needed, and use phototherapy for jaundice. Parents are encouraged to participate through kangaroo care (skin-to-skin contact), which boosts bonding and development.
Equipment plays a crucial role:
Incubators for warmth and protection
Ventilators for breathing assistance
Monitors for heart rate and oxygen levels
Staff, including neonatologists and nurses, work tirelessly, while dietitians ensure proper feeding plans. The focus is on helping babies reach milestones like independent breathing and weight gain before discharge, which can take days to months.
Navigating newborn challenges can be overwhelming, but with the right care, most babies flourish. At Unittas Hospital, our commitment to excellence in neonatal services ensures your little one receives compassionate, top-tier support tailored to their needs. Trust in expert care to turn vulnerable beginnings into healthy futures.
Frequently Asked Questions
How long do most babies stay in the NICU?
Stays vary from a few days for minor issues to several months for very premature infants, depending on their progress.
Can parents visit their baby in the NICU anytime?
Most units allow 24/7 access, but with hygiene protocols like handwashing and limited visitors to prevent infections.
What role do therapists play in NICU care?
Occupational and physical therapists help with developmental milestones, such as improving sucking reflexes or motor skills.
How is pain managed for NICU babies?
Non-pharmacological methods like swaddling are preferred, with medications used sparingly under close monitoring.
Are there support groups for NICU parents?
Many hospitals offer counseling or peer groups to help families cope with emotional stress.
What vaccinations do NICU babies receive?
They get standard immunizations on an adjusted schedule, often starting with hepatitis B right after birth.
How does NICU care affect long-term health?
With proper intervention, most graduates have excellent outcomes, though some may need follow-up for vision or hearing.
Can breast milk be provided in the NICU?
Yes, mothers are encouraged to pump and supply milk, which is fortified if needed for nutritional boost.
What happens during NICU rounds?
Daily team discussions review each baby's status, adjust treatments, and plan for the day.
How do NICUs handle emergencies?
They have rapid response protocols, with on-site specialists and equipment ready for immediate action.
Is music therapy used in NICUs?
Gentle sounds or lullabies can soothe babies, reducing stress and aiding heart rate stability.
What follow-up care is needed after NICU discharge?
Regular pediatric visits, developmental screenings, and sometimes home nursing for ongoing monitoring.
Planning your pregnancy care?
Unittas offers end-to-end pregnancy & maternity packages in Chennai.
Get Expert Care at Unittas Hospital
Our caring specialists are here to guide you through every step with safe, evidence-based care.